Damaged Sperm & Common Chemical Exposure Links to Learning Disabilities, ADD and Behavior Disorders The following is one chapter from a 1997 Graduate Student Research Project conducted at the University of South Florida. The project involved locating published peer reviewed medical journal articles which have shown various environmental and chemical exposure factors can cause learning disabilities, hyperactivity and other disorders by damaging the delicate brain growth process in the unborn child during pregnancy. Author: Richard W. Pressinger (M.Ed.) Sperm Toxicology Index INTRODUCTION 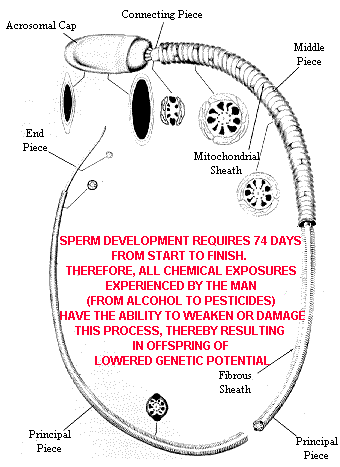
The basic premise is simple - it takes 74 days for the male to make the sperm that will get his partner pregnant (some studies say 65 days). This fact would help explain why men exposed to chemicals on the job or at home for 2 months prior to conceiving have a greater likelihood of their child being born with health disorders. Studies of the father’s role in contributing to increased learning and behavior disabilities in children have received attention only recently. The past 10 years has shown an increase in studies linking weak or defective sperm to employment in occupations with exposure to chemicals and pesticides (American Journal of Industrial Medicine 24:587-592, 1993). Weak or defective sperm are giving evidence of having an increased risk for problems with pregnancy and the offspring. In a statement from researchers, Dr. Hemavathi and Dr. Rahiman of the Department of Biosciences, Mangalore University, India (4),
As an example of this observation, Dr. Hemavathi subjected mice to levels of three common pesticides - ziram, thiram and dithane M-45 in order to observe effects upon the animals’ sperm. Doses were given daily for five days at one-fourth that which is known to kill 50% of the animals. Results showed all the pesticides caused over a 3 to 8-fold increase in sperm abnormalities such as double heads, small heads, elongated heads, large heads, double tails, coiled sperm, and acrosomes (tip of the head) bent upward or downward and some sperm without acrosomes. Understanding of the sequence for male sperm production helps understand the vulnerability of the sperm to environmental/chemical exposures. One common public misunderstanding is that the male manufactures millions of sperm daily, so therefore, activities engaged in weeks or months earlier would then not have an effect upon the sperm quality. This assumption is actually incorrect. Although it is accurate that the human male produces millions of sperm daily, it is important to realize that it takes 74 days to actually create the sperm within the testicles. So therefore, there is over two months worth of time before conception that the male can be exposed to environmental circumstances that could slow or harm the healthy genetic development of the sperm cell. It is now generally accepted that the U.S. male population has shown a large decrease in sperm counts since the 1930’s and 40’s. This in itself does not generate too much concern since conception can occur even with low sperm counts. However, what should generate significant concern is the fact that research reported by several investigators has shown that when low sperm counts are present in various species of animals there is an increase in the frequency of abnormal pregnancies (Damarajan, M. Nature, 165:398, 1950 and Knudsen, O., International Journal of Fertility, 3:389, 1958). Combining the information from both of these investigators then suggests that serious consequences could already be appearing due to the continued decline in male sperm counts in industrialized nations. Miscarriages Linked to Men with Lower Sperm Counts SOURCE: International Journal of Fertility, Vol. 7(1):17-21
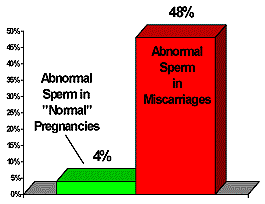
Pregnancies ending in miscarriage were found to have fathers whose sperm showed higher levels of defective sperm as well as lower sperm counts. This was the conclusion in a 1962 research project conducted by the Department of Obstetrics and Gynecology at the Sabbatsberg Hospital in Stockholm, Sweden. Semen specimens were gathered from 201 men whose wives had experienced miscarriages in the second to third month of pregnancy or abortions in the fourth to fifth month of pregnancy. (The term "abortions" in this context was the term used in the early 1960’s to define miscarriages that occurred after the third month of pregnancy). In the research families, over half the families had experienced two or more abortions (late miscarriages). For comparison, a control group of 116 sperm samples were also checked from husbands who had visited the hospital but whose wives had produced living normal children within two years. To insure similar parameters among participants, sperm samples were acquired by masturbation after an abstinence period of five days. Results of the two groups showed that sperm counts for the abortion/late miscarriage group was 110.2 million per cubic centimeter, while the sperm counts for the control group was 138.7 million per cubic centimeter. The investigators classified this as "highly significant statistically." Of even more concern, it was found through microscopic examination of sperm samples that approximately 48% of the sperm were "abnormal" in the miscarriage group while only 4% of the sperm were "abnormal" in the control group who produced normal children. In summary, the researchers stated,
Drs. Mirjam Furuhjelm, Birgit Jonson, and C.G. Lagergren
Sperm Counts Decline Since 1940’s Testicle Abnormalities Increase SOURCE: Environmental Health Perspectives, Vol. 101(2):65-71, 1993 Several biological problems affecting the male testicles have been occurring with greater frequency over the past 50 years. The summary of the problem, which appeared in the 1993 journal, Environmental Health Perspectives, discussed the observed rise in testicular cancer and the medical conditions hypospadias and cryptorchidism, as well as the apparent declining sperm count among the overall male population. According to the researchers at the Statistical Research Unit, University of Copenhagen, Denmark, cancer of the male testicles has increased over 3 fold from 1940 to 1980. The frequency of hypospadias in England and Wales has doubled from 0.15% in 1964 to 0.36% in 1983. Similar increases were also reported from Sweden and Hungary. Recent British data also detected a near doubling of the condition cryptorchidism from 1.6% of the boys born in the 1950’s to 2.9% born in the late 1970’s. The researchers also performed a statistical analysis of the total international literature on semen parameters published between 1930 and 1991. Compiling information from over 61 papers and 14,947 males indicated a significant decline in average sperm density form 113 million per milliliter in 1940 to 66 million per milliliter in 1990. The mean seminal volume also declined from 3.40 milliliters to 2.75 milliliters ( a 0.65 milliliter drop). This means that the total sperm count decreased even more than that expressed by sperm density. In other words, men are producing only about half as much sperm per ejaculation today as they did in the 1940’s. In conclusion the researchers stated,
Aleksander Giwercman, Elisabeth Carlsen, Niels Keiding, and Niels E.
Skakkebaek Fathers' Drinking Lowers Birth Weight of Babies SOURCE: Miami Herald, June 19, 1986, pg. 24a Fathers who were considered "regular" drinkers had babies that weighed over one-third of a pound less than babies whose fathers were only "occasional" drinkers. The study was outlined in the June 19, 1986 Miami Herald and reported in the New England Journal of Medicine. The study was conducted by epidemiologist Ruth Little and Charles Sing at the University of Michigan. As part of the study, the researchers questioned 377 mothers about their drinking and smoking habits before and during pregnancy, and about the drinking habits of their husbands in the month before they conceived. To their surprise, the researchers found that the fathers who drank an average of two drinks a day per month had the lower weight babies. Dr. Little stated,
The research did not investigate whether this loss of weight occurred in the child’s body mass or brain weight. Dr. Ruth Little and Dr. Charles Sing Sperm Damage Suspected from Chemotherapy - Offspring Show Motor Development Disorders SOURCE: Science, Vol. 211(2), January, 1981 Adult rats exposed to the common cancer chemotherapy drug cyclophosphamide produced offspring that showed retardation in various tests of behavior development. The study, conducted by several colleges including the Division of Environmental Toxicology at the University of Texas Medical Branch, conducted behavioral assessments of the offspring using the following procedures.
The rats were injected with the chemical for 5 days, allowed to rest for the next 2 days and then treated again for a period of 5 weeks. Beginning 3 days after the last injection, the animals were housed in cages with a ratio of two females to one male per cage for about 2 weeks. Results of the study showed that there was no significant difference in surface righting ability in the exposed and not exposed rats. However, cliff avoidance was significantly slower for rats whose fathers were exposed to the cancer drug before conception. Swimming ability was also more difficult for the rats whose fathers were exposed to cyclophosphamide. They showed a greater number of offspring who swam with their heads lower in the water. Regarding the swimming direction of the animals, 10% of the non-exposed offspring swam in circles at 10 days of age, whereas over 40% of the exposed offspring swam in circles at 10 days of age. No difference was seen in both groups with the negative geotaxis test. Evidence of hyperactivity was seen in the open-field testing at the age of 14 and 21 days after birth and was considered significant. In conclusion, the researchers stated,
Drs. M. Adams, Jill D. Fabricant & Marvin S. Legator Low Sperm Counts and Infertility More Common in Agricultural Workers SOURCE: American Journal of Industrial Medicine 24:587-592, 1993 Men working in the agriculture industry showed more than a ten-fold increased risk of having infertility in comparison to other job occupations. Investigating their "suspicions" after treating infertile couples, physicians at the Institute of Sterility in Vienna, Austria compared 103 consecutive couples who had sought artificial insemination with donor sperm (abbreviated as AID) and compared their job occupations with 103 couples who had sought help due to female fertility problems. The researchers reported that the patients medical histories showed no indications that diseases, long-term medication use, or cigarette smoking was related to male infertility. In explaining their observations the investigators stated,
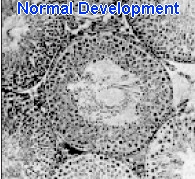
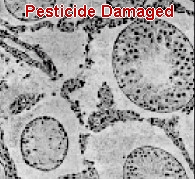
Dr. H. Strohmer, M.D., Andrea Boldizsar, MD, Barbara Plockinger, MD Pesticide Causes Testicle Damage Reduces Sperm Counts SOURCE: Bulletin of Environmental Contamination Toxicology 55:1-7, 1995 As reports of infertility among pesticide workers are increasing (3), researchers at Kyushu University, Japan investigated the effects of the nematode pesticide DBCP (dibromochloropropane) and several related industrial chemicals called DC1P (dichoro-1-propanol) and DC2P (dichloro-2-propanol) along with the metabolites of these chemicals (metabolites are the new compounds resulting after the liver metabolizes the original compound). The metabolites investigated were ACH (alpha-chlorohydrin) and ECH (epichlorohydrin).
Results showed that sperm counts were significantly reduced in the DC1P and DC2Pgroup and animals exposed to the pesticide DBCP showed a drastic reduction in sperm counts in comparison to the normal controls. The animals exposed to the ACH metabolite also showed a slight but significantly reduced sperm count. Regarding the morphology (shape) of the sperm, there were not significant differences among any of the groups except a drastic increase in sperm without tails in the DBCP group. Whereas, there were only 14 per 1000 sperm with missing tails in the control group, there were 865 per 1000 sperm with missing tails in the DBCP exposed animals. Such a drastic paralysis to sperm certainly explains the resulting infertility from these chemicals. Drs. M. Omura, M. Hirata, M. Ahao Surprising Testicle/Sperm Abnormalities Appear After Consumption of Chemically Grown Foods SOURCE: Journal of Reproductive Fertility, 1:130-138, 1960 In the early 1960’s when farming was making its switch away from naturally growing methods to the now common chemical fertilizer/pesticide growing methods, investigators were concerned of the effects such foods might have on human health. To study the effect chemically grown foods would have on general health and the reproductive system, researchers at the Royal Free Hospital School of Medicine in London conducted an experiment in which 3 groups of 17 pairs of mice were fed wheat that was grown using either one of the following three different methods: Group 1 - Chemical Fertilizers Alone (called "stockless") Group 2 - Chemical Fertilizers & Manure (called "mixed") Group 3 - Organically Grown using compost (called "organic")
The researchers stated that wheat in itself is not the best food for mice, however, the results do show that - CHEM-TOX COMMENTS: Why does this happen? Although scientists did not address this specific question - there are several points that should be considered. #1 -
REPRODUCTIVE SYSTEM HIGHLY VULNERABLE TO PESTICIDES #2 - LOWER
TRACE MINERAL CONTENT IN "CHEMICALLY-GROWN" FOODS Dr. Patricia P. Scott,
J.P. Greaves and M.G. Scott
Anesthesia Suspected in Abnormal Sperm Development Problems in spermatogenesis in mice has also been found to occur after exposure to common anesthesia enflurane (Land et al., 1981). Morphologic changes were observed in mouse spermatozoa after exposure to inhalation anesthetics during early spermatogenesis. (details of this study to be posted soon) Anesthesiology 54:53-56, 1981 Additional References |